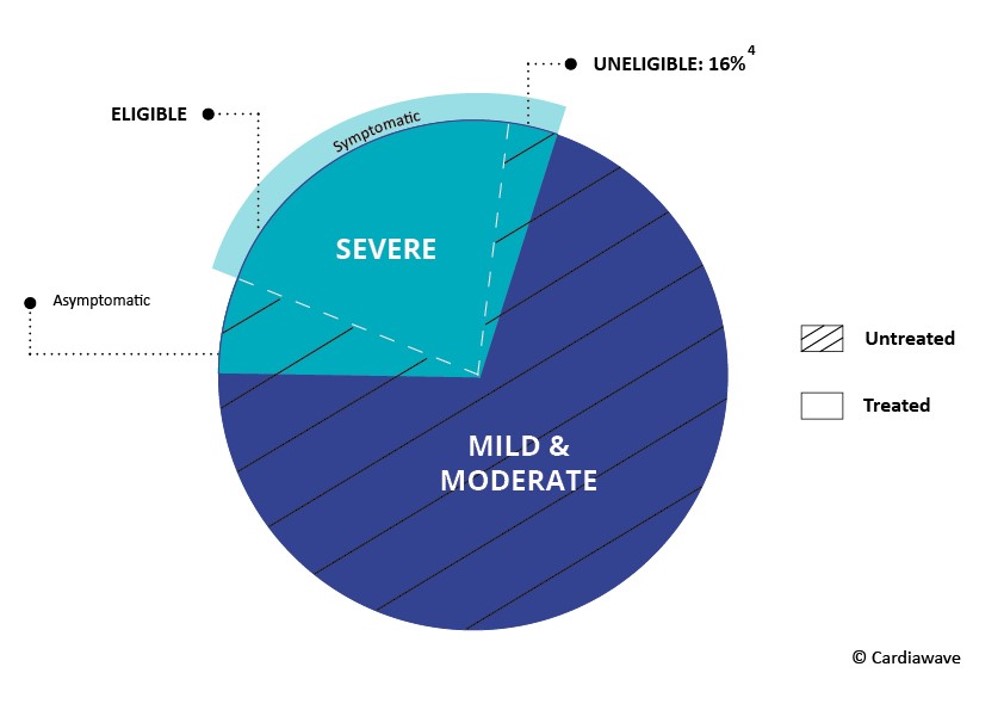
Aortic stenosis (AS) is one of the most common and serious valve disease problems. It is a life-threatening disease caused by the narrowing of the opening of the aortic valve. It is made up of three flexible leaflets that need to open completely to allow oxygened blood to exit from the heart towards the vital organs. AS restricts the blood flow from the left ventricle to the aorta.
In developed countries, AS is the third-most frequent cardiovascular disease (1) (2). AS affects 1,7% of the population aged 65 and over and 12,4% of people over 75 (1) (2) (3) : it has become a major public health concern because of the ageing Western population. The number of elderly patients with severe AS in North America is expected to increase from 540,000 patients in 2012 to 800,000 (+8.3%) in 2025 and 1.4 million (+11.8%) in 2050 driven by ageing population and better diagnosis(3). The average life expectancy of patients with severe, symptomatic AS is only 2.3 years without aortic valve replacement with a significant risk of sudden death (4). 65% of severe symptomatic AS patients remain untreated in the United States of America (5).
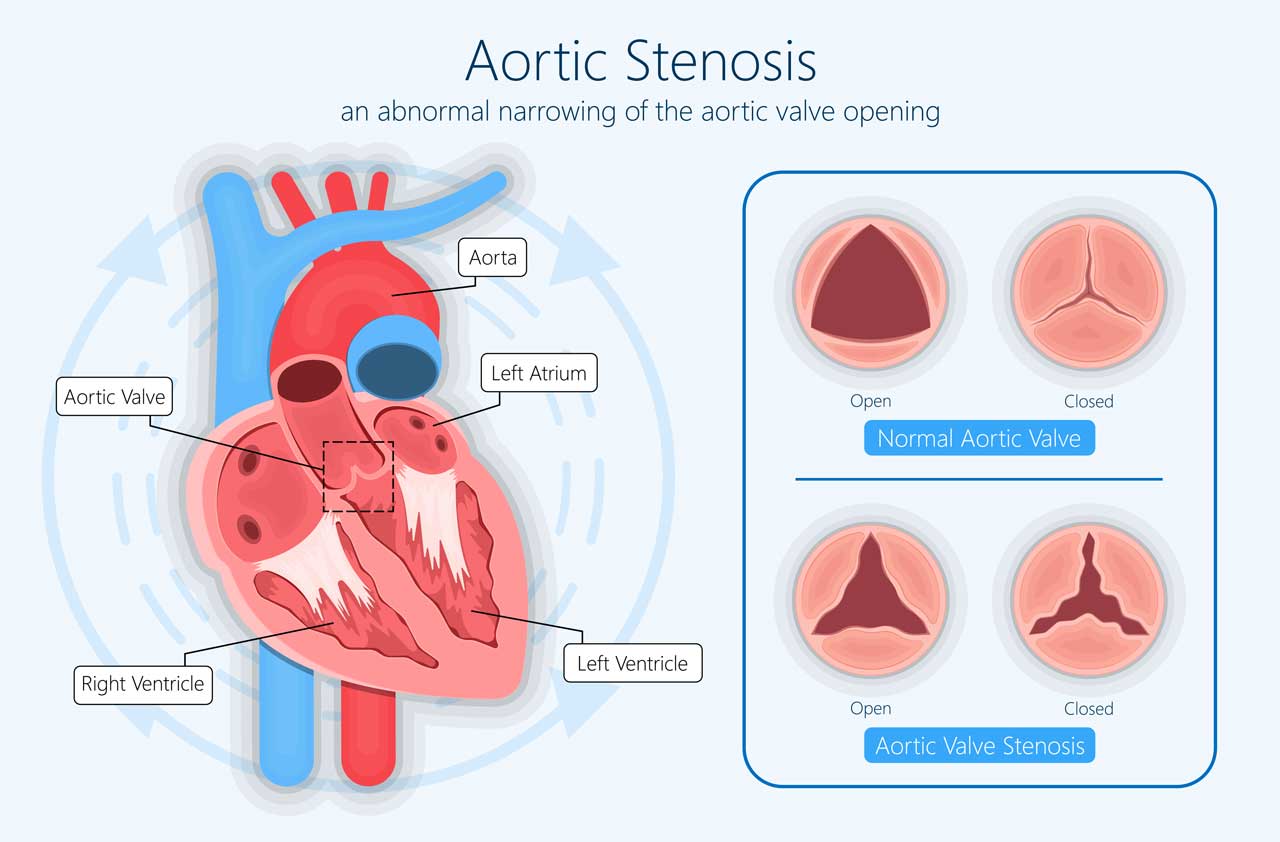

Severe symptomatic, severe Calcific Aortic Stenosis (CAS) is associated with significant morbidity. Once symptoms appear, untreated patients have a poor prognosis; they will experience worsening symptoms, eventually leading to death. After the onset of symptoms, average survival is 50% at two years and 20% at five-years (1). The standard of care (SoC) for severe symptomatic CAS is currently invasive. Even after less-invasive treatment, mortality is still 2.27% after one month and 11.35% after 1 year (2).

These procedures represent a significant cost to public health systems. Heart valve disease costs the U.S. US$23.4 billion each year in direct health care expenditures. Symptomatic aortic valve disease costs the U.S. at least US$5.6 billion in direct health care expenditures each year (1).
Many patients untreated
In spite of the Transcatheter Aortic Valve Replacement (TAVR) revolution, Aortic Stenosis (AS) is still an unmet medical need. Most of the patients remain untreated.
International guidelines (1) (2) recommend nowadays to treat patients affected with severe symptomatic AS. 65% of severe symptomatic AS patients remain untreated in the United States of America (3) due to absence of diagnosis, lack of infrastructure, restrictions from payers or costs of aortic valve replacement.
All other patients evolving to a severe stenosis are not treated because they have no treatment options: huge unmet medical need.